Food Deserts
Many low-income communities and rural neighborhoods across the U.S. live in what are known as “food deserts,” where there is little or no access to healthy foods. Instead, within reach are fast food chains and small, local convenience and corner stores that have limited fresh produce, sell fatty, processed foods, and have ample sweets and snacks. Often without cars or convenient public transportation, people are forced to rely on these foods, which can contribute to a poor diet and lead to higher levels of obesity and other diet-related illnesses, such as diabetes and heart disease. This is an example of how individual eating behaviors are shaped by factors in social and physical environments.

Courtesy of The White House, Washington, D.C.
https://youtu.be/8My-iWjTBQ8
In this 2010 video, First Lady Michelle Obama outlines an ambitious campaign to eliminate food deserts in the U.S. by leveraging federal dollars with commitments from local and state governments, industry, and non-profit organizations.
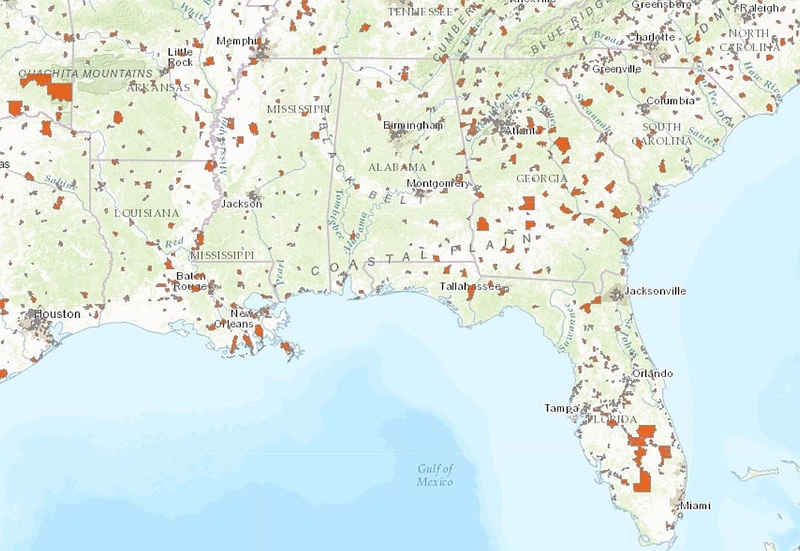
Produced by the United States Department of Agriculture (USDA)
https://www.ers.usda.gov/data-products/food-access-research-atlas/
Produced by the United States Department of Agriculture (USDA), the Food Access Research Atlas allows the user to investigate food store access, nationwide.
This still from the atlas shows low-income areas with at least 500 people (or 33 % of the population), living more than 1 mile (urban areas) or, if in rural areas, more than 10 miles from the nearest supermarket, supercenter, or large grocery store.
Further Reading
Carnahan, L. R., Zimmermann, K., & Peacock, N. R. (2016). What Rural Women Want the Public Health Community to Know About Access to Healthful Food: A Qualitative Study, 2011. Preventing Chronic Disease, 13, E57.
Leone, A. F., Lee, J. S., Rigby, S., Kurtz, H., Johnson, M. A., Betterley, C., & Park, S. (2011). Store Type and Demographic Influence on the Availability and Price of Healthful Foods, Leon County, Florida, 2008. Preventing Chronic Disease, 8(6), A140.
Valdez, Z., Ramírez, A. S., Estrada, E., Grassi, K., & Nathan, S. (2016). Community Perspectives on Access to and Availability of Healthy Food in Rural, Low-Resource, Latino Communities. Preventing Chronic Disease, 13, E170.